Archive
Medical Technology Update – The OmniPod 5
One of the more interesting psychological challenges I’ve had during my time as a diabetic has been an underlying belief that any change in treatment was to be considered a failure. When you are actively managing an illness in the way diabetes requires, your vigilance, resilience, and willpower are constantly at risk. For quite a while now I’ve resisted the idea of using an insulin pump rather than giving myself 4 to 5 injections a day; it felt like all of the effort I’d put in the last several years to get myself basically “normal” blood sugar wise just hadn’t been enough, and that I’d still failed.
This was especially true early in my battle, before 2018, when I found a new doctor and was first exposed to continuous glucose monitoring systems such as the Dexcom I still wear to this day. I’ve spoken about this in two earlier blog posts, one from that period in 2018 and one earlier this year that updated my technology usage and its success. Before that, cycling through doctors and medications and periods of simply bad health had left me feeling as though I was in a losing battle.
That feeling can be hard to shake even when one succeeds for a sustained period of time.
For the past few years my doctor, who is incredible, has asked about possibly using an insulin pump. There are several benefits, including no longer needing to carry insulin pens when out and about. I had always resisted because of the seeming permanence of a device, as well as the psychological acknowledgement that we’ve crossed another line in our defense, potentially the last line. One step closer to failure. In addition, most modern insulin pumps require tubes, and that just felt…overreaching.
Two months ago at my quarterly check in, my doctor again asked about using a pump, and mentioned there was a new kind of pump that was compatible with my Dexcom and did not use tubing. The OmniPod 5, while relatively new, was constructed for people with both Type I and Type II Diabetes.
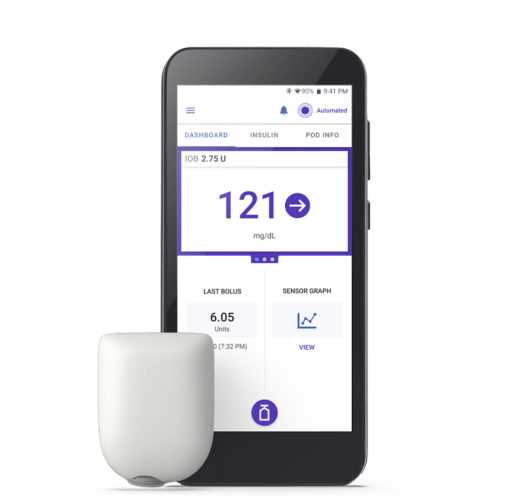
With my success with the Dexcom, the compatibility of the OmniPod with my Dexcom, the smallish profile of the device, and the lack of tubing, I finally decided to take a shot at using an insulin pump.
What a game changer.
Although learning how to apply the device requires a training session, once you have it down, application is relatively easy. The device is a bit larger than I expected, but it’s light and once you’re used to it it’s not too bad. The biggest adjustment has been sleeping on it without feeling like you’re pushing it. The insertion of the needle is quick and relatively painless. I flinch at times but it’s no worse than a normal insulin injection. The pods last about 3 days, so you’re replacing them often, but what it solves is permanent availability of insulin without needing pens or needles.
I haven’t missed a pre-meal insulin in the first three weeks of using this device. It uses AI and an initial dosage from my doctor, giving me a few units every hour as a maintenance dose, and then I can override as needed. I never have to interrupt myself to inject insulin. I control the device right from my iPhone, making eating meals out as easy as eating at home. The device effectively removes any reason to not be on top of my insulin levels every waking moment.
The results are astonishing. My average glucose level has gone down from ~140 to ~115. My in range Dexcom readings went from ~80% to ~98% in range; I went seven consecutive days at one point without a single Dexcom reading outside of my high or low range parameters.
My projected A1C has dropped from 6.9 to 6.1. That’s basically normal for a healthy human.
There are a few cons with this. I mentioned the device size, and sleeping adjustments, but I’ve made those. Changing every three days or so has been manageable. The one thing I don’t particularly like is having it on the same arm that my Dexcom is on; the bluetooth connections between my Dexcom and Omnipod aren’t strong enough to work unless they are within a few inches of each other. In addition, because the needle is a bit bigger than what the Dexcom uses, I am actively rotating positions, which means I’m alternating left and right arms as I change Dexcom sensors. The device is also big enough to be obvious in short sleeves, so I’ve taken to wearing long sleeves just to keep myself from being too self-conscious.
These “cons” are really minor inconveniences that don’t outweigh the major benefits of not having to carry insulin with me, not having to interrupt life to go take shots when I’m out or even when I’m home, and my ability to manage my insulin levels from my phone.
I suppose the moral of the story is don’t let your fear of failure interfere with success….but it could also be that everything is worth a try. In any case, I’m glad I was able to recognize when the parameters of trying a pump made sense to me personally, and I’m feeling very positive about my future as a diabetic.
Medical Technology Update
This week marks the 24th anniversary of my diagnosis as a Type II diabetic. The first 15 years were marked with difficulties maintaining my weight, diet, and a consistent blood sugar level. That all changed in 2018 when I switched doctors to an endocrinologist at Sansum Clinic in Santa Barbara. At the same time, the first iterations of continuous glucose monitors hit the commercial market.
Both events changed my entire outlook on how I managed my disease. I wrote about the impact of the first Dexcom device on my health in a post in 2018. At the same time, my doctor was really what I needed at the time. My very first diabetes doctor was a wonderful lady from Europe, but once I moved to the Central Coast, I struggled to find a doctor who had the right approaches to handle my condition. Switching to my endocrinologist was a literal lifesaver, as he worked with me to find treatments that worked rather than simply talked at me about what I should be doing.
And over the last eight years, the medical technology has continued to advance, leading to an unprecedented string of success in my management of my disease. One would think that over time success would slowly degrade, but the last two years I’ve managed to hit my best numbers yet, and maintain them.
For those of you who aren’t aware, the way diabetes is measured is by measuring the average volume of glucose in the blood stream over the trailing 3 month period. This measurement, the HbA1c (Hemoglobin A1c), is tested routinely every appointment. The HbA1c’s normal range is between 5.5 and 6.5, with anything over 7 considered to be diabetic. My target number in my head is 7 or lower. For historical context, when I began using a Dexcom, my HbA1c was a staggering 12.
This measurement is different than what the Dexcom measures, which is a point in time measurement of glucose volume in the blood stream. That normal range is between 80 and 120, and is the numeric value that appears on Dexcom’s monitoring app. For historical context, when I was diagnosed I was at an unfathomable 549.
As I mentioned in my previous post, which is worth a read, one of the things constant feedback allows is for the patient to have full visibility into how their blood is reacting at any point in time; I’ll admit at this point I understand way more about my blood chemistry than I ever wanted to learn. But the constant feedback allows for targeted action with insulin and diet.
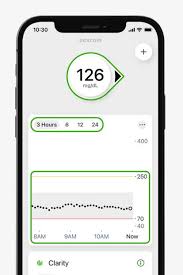
The current device, the Dexcom G7, has come leaps and bounds in terms of reliability and accuracy. The device used to take hours to “warm up”; now readings after sensor application are available in about 20 minutes. The device used to be on the abdomen and could awkwardly catch on things, but now I wear it on the back of my upper arm. The applicator is easier to use, with a simple push button mechanism. And the technology on the phone has advanced to the point where it can extrapolate what my HbA1c will be based on its trailing 3 month data.

What this has meant for me is, I no longer fixate on what’s happening right this moment. I react to the changes in my blood chemistry as best I can, but I can also let things go from time to time, such as around the holidays. And this is because my target now is an average glucose level of around 130-140, which according to the application, loosely translates to a 7 on the HbA1c scale. That’s led to less worrying and less stress, allowing me to essentially push and pull on my readings as life happens.
This has been helped by updates to my medications, which are extensive. The biggest impact has been Mounjaro, which is a once a week injection that targets the blood sugar while also having the side effect of appetite suppression. Medications like Mounjaro, Ozempic, and Trulicity have been used for weight loss and have been advertised extensively in that manner, but their impact on diabetes can’t be overstated. I’ve dropped about 20 pounds and maintained that weight loss alongside the technology improvements that manage my life.
As a result, my HbA1c been under 7, and at times as low as 6.5, for two years running now. And to be fair, with less emotional burden or mental stress. Even at times like now, where the holidays have just wrapped up and I’ve had to deal with issues surrounding my job, I still managed to land a 6.8 for my trailing three month HbA1c score. I don’t fist pump often, but when I do, that’s the kind of thing that makes it happen.
And the improvements continue. Dexcom is coming out with a 15 day device (the current one lasts 10 days), which will reduce cost and make it that much simpler to use.
It hasn’t been easy managing my illness, but with all this assistance from my amazing doctor, medications, and technology, the last 2 years out of the last 24 have been the best so far.
When medical technology succeeds
For those of you aren’t aware, I’ve had Type II Diabetes since before my diagnosis in 2002. That’s 16 years so far of medications, finger pricks, blood tests, and constant stress in the back of my mind about my health. I’m medically disposed to such a disease, with my New England food tastes and diet and a genetic disposition towards conditions such as this. For reference, on the day I was diagnosed, my blood sugar level was 459. Normal is 120. So suffice it to say I’ve got it pretty bad in that regard.
For the first 12 years of my diagnosis, I treated my condition with a combination of moderate diet control (I struggle with this to this day, I admit), monitoring of my blood sugar level through finger prick tests 3-4 times a day, and a variety of different medications with a litany of side effects, including various bathroom issues I won’t elaborate on, and a general feeling of lethargy and discomfort. Not to mention some of the worst nighttime leg cramps I’ve ever experienced. It’s no fun going from dream sleep to standing next to your bed stretching out a locked up calf in 2 seconds flat.
By 2014 I’d stopped taking my medications regularly. I realize most people will question this decision but I felt so much better when not on them. The cramps stopped, the various other issues stopped, and I felt healthy and normal. The medications that treated my diabetes that kept me healthy simply made me feel sick all the time. I was growing increasingly frustrated with my inability to control my blood sugar in the absence of my medications and began to not care about that either. I generally consider myself to be an intelligent person, so I understand the consequences of my decision at the time, but to be fair, it was an emotional one built around 10+ years of trying to manage a disease the required me to be constantly vigilant and feel like I just wanted to be in bed all the time.
In 2015 I was running an A1C of over 12, twice the normal level. I asked my primary care physician to recommend a specialist and he referred me to a clinic in Santa Barbara for treatment. My new specialist approached my mental state, which was beyond frustration at this point, by simply asking me what I felt I needed to do to make things better. We agreed to immediately go off all of the medications that were making me feel ill (for the record, metformin is an evil thing) and switch to insulin for full treatment. That helped a great deal, getting back down to an A1C of 7.5 within six months. Additionally, I’ve tried several new medications, some that use the kidneys or liver to filter out high blood sugars, with pretty successful results.
The biggest frustration though was my inability to determine how successful I was in managing my illness. Let’s take the finger prick blood tests as an example. I’m about to have dinner, I take my blood, and it’s 160. I’m going to decide to inject insulin, and I need to decide how much. How do I decide? 160 as a number doesn’t mean anything. It doesn’t tell me if I’m going up or down. It has no context. So what do I do now?
On top of that, let’s say I’m at 185, but I think I’ve had a good day overall. I ate well in the morning, woke up at 115, and I’ve been doing well (or so I thought). I would expect to be maybe 130, see 185, and wonder how that happened, and get super frustrated at what looks like a failure. Running into that day after day gets very discouraging and frustrating. You wonder why you’re trying at all.
Which brings me to the biggest change in my treatment. I agreed to try a continuous glucose monitor, an injectable monitoring device that provides real time constant feedback on where my blood sugar levels are. I currently use the G5 by Dexcom. It’s the little square device in the lower left of this image.

So, first things first. Applying this device is fairly simple. It is no more or less painful than an insulin injection and uses medical adhesive to attach to my left side. It works by injecting a small, needle-thin sensor underneath the skin. Once there, I barely notice it at all, until it’s time to remove it, which is much like any band aid. It’s impossible to notice underneath my shirt and very easy to forget.
What it gives in return is clarity on where I am at any given moment. It takes that 185 I had before and tells me two things. First, whether I am going up or down, and second, how quickly that transition is happening. A 185 coming down quickly from a high number due to a big lunch is a big difference between a slow rise up to 185 that may not level off any time soon. The device checks my readings every couple of minutes, and I can spot trends in my blood sugar level immediately.
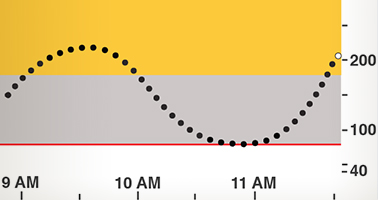
This allows me to thoughtfully examine my daily routine. I can watch my sugar levels after meals, or after snacks, and gain an understanding of the impact of certain foods on my bloodstream In addition, I can intelligently target my insulin levels when I do inject before meals. Before, 185 might mean 10 units of medication. But now, a 185 on its way down might mean 5, but a 185 that’s either level or rising right before I sit down to dinner at Olive Garden might mean 20 units (or a salad instead of pasta). Trends allow me to change behavior on the fly, and react quickly to changes in my blood levels. It’s an amount of control you don’t have when only checking a few times a day, and a way to make sure you have a firm grip on your situation and control over what the number means.
This reduced my stress and frustration level significantly.
Further, there’s an app for my phone that I sync to the device. This not only allows me to track levels, but it will alarm when I go out of a healthy range. There was a period of time where I would have instances of very low blood sugar at night. I’d wake up shaking and sweaty and have to stumble downstairs to grab a drink and a snack to counteract the low blood sugar. But the device will set off an alarm if I start to fall too low, and can warn me before it gets too bad…getting me out of bed before I become possibly too weak to move. You can also set alarms on highs if you want to be notified that you might need an injection or maybe eat less. So with a glance, I can check my phone and see where I am at at any point of the day.
There have been a few challenges. In theory the device can go anywhere on either side of the abdomen, and you are supposed to rotate its location. But I’m a bit on the hairy side as far as body hair, and for some reason, it never stays attached to my right side, so I keep it always on my left. There was the time I hit it getting out of the van and ripped it off, but beyond the surprise, that was no worse than a bad band aid removal.
It says it is waterproof but I haven’t tried that yet. I shower with it but take it off when I swim, which limits my swimming to one day on the weekend. And finally, it’s not supposed to go through any sort of MRI or metal detector, so I don’t take it with me when I travel. I had a notably bad incident in Austin trying to wear it through TSA, and it’s not necessarily worth the trouble to try and get it through security.
But to be clear, in particular if you are accustomed to giving yourself injections, there’s no reason not to try a CGM. I can tell you for sure it’s made managing my disease much more tolerable, and when I do have periods of frustration, it’s a lot easier to slap a device back on and get back on the routine. It’s reduced my overall blood sugar levels by 60% since I’ve started using it. I recommend it for sure.
All images copyright Dexcom (https://www.dexcom.com/)
